Quick Summary
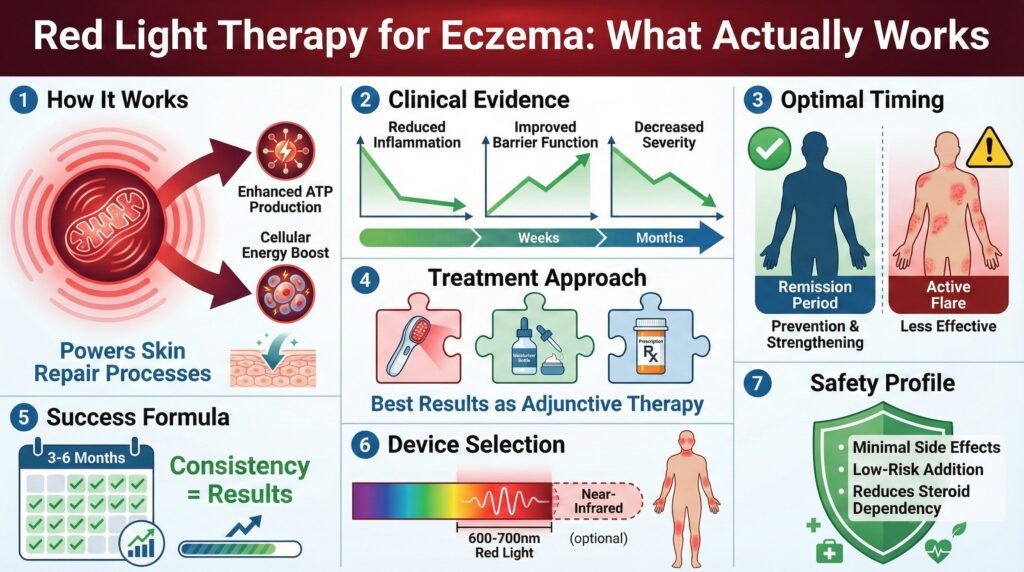
Red light therapy (primarily 600–700 nm) can help manage eczema as a safe, complementary treatment by boosting cellular energy (ATP), reducing inflammation, modulating cytokines, and strengthening the skin barrier.
Clinical studies show 30–40% reductions in eczema severity scores (SCORAD), better barrier function, and symptom improvements with consistent use over weeks to months. Best during remission, not active flares.
It has zero documented side effects in trials, works synergistically with standard treatments (moisturizers, meds), but requires proper devices, dosage, and patience. At-home options (like Kineon) are promoted as cost-effective alternatives to clinic sessions.
Table of Contents
- Introduction: Overview of red light therapy’s potential role in eczema management.
- Understanding Photobiomodulation at the Cellular Level: How red/near-infrared light interacts with mitochondria, increases ATP, reduces inflammation, and supports skin repair.
- The Clinical Evidence That Changed My Perspective Summary of human trials, including an 81-patient study (weekly 2-min sessions), cytokine modulation (2024 research), 30–40% SCORAD reductions, and barrier function improvements.
- When Timing Makes All the Difference. Best used during remission for prevention and barrier strengthening, avoid during active flares to prevent irritation.
- Setting Up an Effective Protocol Recommended wavelengths (600–700 nm red + optional near-infrared), frequency (2–4×/week, 10–20 min), power density (20–40 mW/cm²), distance, and device types (handheld, masks, panels).
- Combining Red Light with Existing Treatments: Synergistic benefits when paired with moisturizers, immunosuppressive meds, wet wraps, etc., for faster/better results.
- Common Mistakes That Undermine Results: Inconsistency, low-powered devices, using during flares, unclean skin, and poor application technique.
- Key Takeaways Core summary: effective adjunctive therapy with strong evidence, no side effects, requires consistency and proper setup.
- People Also Asked FAQ section addressing common reader questions.
Introduction
You’d think something as simple as shining a red light on inflamed skin would either be finished nonsense or a secret cure. But reality, as usual, sits somewhere in the frustratingly complicated middle.
That tension fascinates me.
What drew me into this topic wasn’t the marketing hype. It was actually a conversation with someone who’d struggled with eczema for decades and had tried literally everything, the prescription rotation, the elimination diets, the countless moisturizers that promised barrier repair.
She mentioned casually that a dermatologist had suggested trying red light therapy, not as a replacement for her medications, but as something that might help strengthen her skin between flares.
That specificity caught my attention. Not a cure. Not a replacement.
Just a tool that might help with a particular aspect of a complicated condition.
Understanding Photobiomodulation at the Cellular Level
The mechanism behind what red light therapy actually does isn’t mysterious or magical. When specific wavelengths of light, typically between 600 and 700 nanometers, hit your skin, they penetrate past the epidermis and reach cells in the dermis.
These wavelengths get absorbed by chromophores, particularly cytochrome c oxidase in your mitochondria.
Here’s what happens next, and this is where it gets really compelling. That light absorption triggers a cascade that increases ATP production.
Your cells essentially get an energy boost.
With more available energy, they can perform repair functions more efficiently.
For skin cells dealing with the chronic inflammation and barrier dysfunction that defines eczema, this extracellular energy translates into enhanced capacity for tissue regeneration, collagen synthesis, and ultimately, barrier restoration.
What makes this different from topical treatments is the delivery method itself. You’re not adding a substance to inflamed, compromised skin. You’re not introducing a potential irritant or allergen.
You’re essentially giving cells the energetic capacity to do what they’re already trying to do: repair themselves.
That distinction matters tremendously when you’re dealing with skin that reacts to seemingly everything.
The research on this mechanism has progressed significantly over the past decade. We’re not talking about preliminary cell culture studies anymore.
Multiple human clinical trials have documented measurable changes in inflammatory markers, skin thickness, and barrier function metrics after consistent red light exposure.
The wavelength specificity matters more than you might think. Red light in the 600-700 nanometer range penetrates to different depths than other wavelengths.
Too short, and you’re only affecting surface cells.
Too long, and you’re entering infrared territory with different biological effects. The sweet spot for eczema appears to be that classic red light range, though near-infrared wavelengths between 700-1100 nanometers may provide additional anti-inflammatory benefits in deeper tissue layers.
The mitochondrial response happens quickly. Within minutes of light exposure, you can measure increased ATP production in treated cells.
But the downstream effects on barrier repair, inflammation reduction, and tissue remodeling take much longer to manifest in ways you can actually see and feel.
This delayed manifestation is why so many people give up too early. They expect to see results within days when the actual biological processes require weeks to months of consistent application.
This is why red light therapy demands consistent use multiple times per week. When relying on professional clinical sessions costing $75 to $125 per session, this can add up.
Hence, the need for a reliable and effective at-home red light therapy device is key. To get a better idea, use the cost-savings calculator below to crunch the real numbers, and a link to Kineon’s catalog of affordable red light devices.
💰 Red Light Therapy Savings Calculator
Discover how much you can save with Kineon’s at-home red light therapy compared to professional clinic sessions. Get professional-grade treatment from the comfort of your home.
The Clinical Evidence That Changed My Perspective
I used to be pretty skeptical about light-based therapies outside of prescription phototherapy with narrow-band UVB. Then I came across a clinical trial that really shifted my thinking.
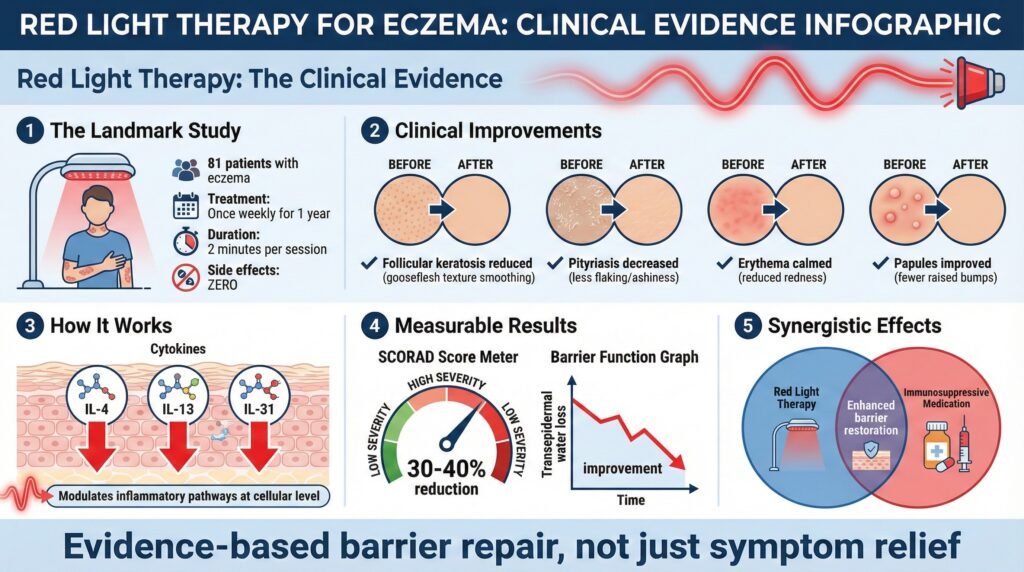
Eighty-one patients with eczema received red light therapy once per week for nearly a year. Just once per week. And each session lasted only two minutes.
That minimal intervention protocol produced documented improvements in follicular keratosis, the rough, gooseflesh-like texture that appears with chronic eczema.
It reduced pityriasis, the flaking that makes skin look ashy and feel rough.
Erythema decreased, meaning the angry redness that signals active inflammation calmed down.
Even papules, those raised, inflamed bumps, showed improvement.
What struck me most wasn’t just that these improvements occurred. It was that they occurred with such minimal treatment frequency and with zero documented side effects.
When you compare that safety profile to systemic medications or even long-term topical steroid use, the risk-benefit calculation starts looking really different.
Another study combined red light with an immunosuppressive medication and found that the combination restored skin barrier function more effectively than either intervention alone.
That synergistic effect suggests something important: red light therapy might work particularly well as part of a comprehensive protocol as opposed to as a standalone intervention.
More recent research from 2024 explored how red light affects the inflammatory cascade at a molecular level. The findings showed modulation of pro-inflammatory cytokines, those chemical messengers that drive the itch-scratch cycle and perpetuate inflammation.
This wasn’t just surface-level symptom reduction. The light was influencing actual immune signaling pathways.
The cytokine modulation aspect is particularly interesting because it addresses one of eczema’s core problems. In atopic dermatitis, you typically see elevated levels of Th2-associated cytokines like IL-4, IL-13, and IL-31.
These cytokines drive the inflammatory response and contribute directly to itching.
Red light exposure has been shown to reduce these specific cytokine levels while potentially supporting regulatory immune responses that help calm inflammation.
Studies measuring SCORAD scores, a standardized assessment tool for eczema severity, have consistently shown statistically significant reductions after weeks to months of regular red light therapy.
These weren’t marginal improvements. Some studies documented 30-40% reductions in overall SCORAD scores, which represents a meaningful improvement in quality of life for people dealing with chronic eczema.
The transepidermal water loss measurements tell another important part of the story. This metric directly assesses barrier function, how well your skin keeps moisture and keeps irritants out.
Multiple studies have documented measurable improvements in transepidermal water loss after consistent red light therapy, indicating genuine barrier repair as opposed to just temporary symptom relief.
When Timing Makes All the Difference
One of the most practically important insights about red light therapy for eczema involves timing.
Most people intuitively think you should use treatments when symptoms are worst, during active flares when skin is red, inflamed, and unbearably itchy.
But dermatologists who work with LED therapy consistently recommend the opposite approach.
Red light therapy works best during remission periods, when your skin has calmed down, and you’re not in the middle of an acute inflammatory episode. During flares, your skin barrier is severely compromised. You’ve got increased transepidermal water loss, heightened sensitivity to irritants, and an already overactive immune response.
Introducing any intervention during that vulnerable state carries the risk of additional irritation.
But during remission, when inflammation has subsided, but your barrier function is still impaired, red light therapy can help strengthen that barrier proactively. Think of it as preventive maintenance as opposed to emergency repair.
You’re supporting the skin’s natural healing processes when it’s actually capable of responding to that support.
This timing distinction also explains why some people report that red light therapy “doesn’t work” for their eczema. If they tried it during active flares and experienced additional irritation or saw no immediate improvement, they understandably concluded it was ineffective.
But they were essentially using the right tool at the wrong time.
The preventive application makes even more sense when you understand eczema’s chronic, relapsing nature. Most effective long-term management focuses heavily on preventing flares as opposed to just treating them once they occur.
Red light therapy fits naturally into that preventive framework.
The biological rationale for this timing approach becomes clearer when you consider what’s happening at a cellular level during flares versus remission. During active inflammation, your immune system is already in overdrive.
Mast cells are degranulating, releasing histamine and other inflammatory mediators.
Your skin is flooding with immune cells. Adding any stimulus, even useful light, to this chaotic environment can sometimes trigger additional reactivity.
During remission, your skin’s inflammatory state has normalized enough to respond productively to stimulation. The cells can actually utilize that increased ATP production for repair processes as opposed to fighting active inflammation.
Setting Up an Effective Protocol
Starting red light therapy for eczema requires more strategic thinking than just buying a device and shining it on your skin daily. The research that showed positive results used specific parameters, and replicating those parameters matters if you want similar outcomes.
Wavelength selection comes first. You’re looking for devices that emit light in the 600-700 nanometer range for red light, or extending into 700-1100 nanometers if you want near-infrared as well.
Near-infrared penetrates deeper and may offer additional benefits for inflammation reduction in the dermis. Some evidence suggests combining both wavelengths produces better results than either alone, though the research on optimal combinations is still evolving.
Treatment frequency seems to follow a dose-response relationship up to a point. The minimal protocol from that year-long study was once weekly for just two minutes.
But other research using more frequent applications, three to four times per week for 10-20 minutes, showed more rapid improvements.
You’re balancing consistency against the risk of overdoing it, especially when you’re first establishing tolerance.
I’d suggest starting conservatively, maybe twice weekly for 10 minutes, and gradually increasing frequency as you confirm your skin tolerates the exposure well. Some people can handle daily treatments without issue.
Others find that every other day works better for their particular skin reactivity.
Distance from the light source affects intensity. Most at-home red light therapy devices work best at 6-12 inches from the skin, but always check your specific device’s recommendations because power output varies considerably between products.
Device format matters based on where your eczema appears. Full-face masks work well if you have facial eczema, but they expose healthy skin unnecessarily if your problem areas are localized.
Handheld wands give you more control for targeting specific patches on arms, legs, or hands. Read our review of Quasar MD’s handheld devices here.
Larger red light panels make sense if you’re dealing with extensive body involvement.
Power density is one of the most overlooked factors when people buy devices.
You want at least 20-40 milliwatts per square centimeter at your treatment distance for effective therapy.
Lower-powered devices might still provide some benefit, but you’d need to extend treatment times significantly to deliver comparable light energy to your cells.
The irradiance, which is the power density reaching your skin, decreases with distance. If a panel delivers 40 mW/cm² at 6 inches, it might only deliver 20 mW/cm² at 12 inches.
That’s why following manufacturer guidelines for distance matters so much.
Combining Red Light with Existing Treatments
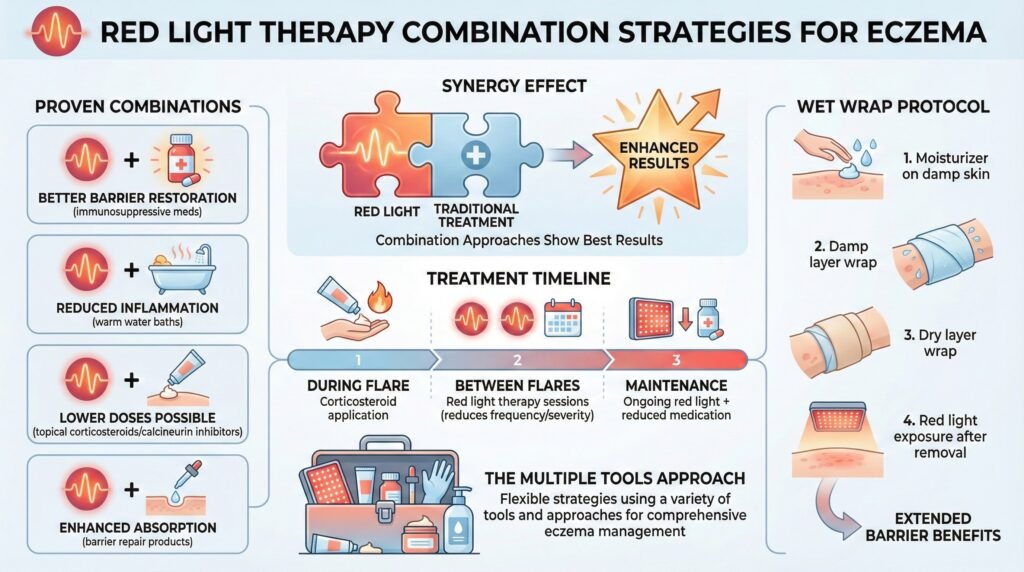
The research showing the most impressive outcomes often involved combination approaches. Red light paired with immunosuppressive medications produced better barrier restoration than either treatment alone.
Red light combined with simple warm water baths reduced inflammation and suppressed allergic reactions more effectively than baths alone.
This synergistic pattern suggests that red light therapy excels as an adjunctive treatment, something that enhances and supports your primary interventions.
If you’re using topical corticosteroids during flares, continuing red light therapy between flares might reduce flare frequency or severity.
If you’re on a maintenance regimen with topical calcineurin inhibitors, adding red light might allow you to use lower doses.
There’s also practical value in having multiple tools available. Eczema management often requires adjusting your approach based on what’s happening with your skin at any given time.
Having red light therapy as an option gives you another lever to pull when you’re trying to maintain remission or support healing after a flare subsides.
Some dermatologists suggest applying serums or barrier repair products before red light therapy sessions, reasoning that the increased cellular activity might enhance absorption and efficacy. The evidence for this specific protocol isn’t strong yet, but the logic is sound enough that it’s worth experimenting with if you’re already using both interventions.
The concept here is that enhanced cellular metabolism might increase uptake of useful ingredients. Your cells are in a more active state, potentially more receptive to the ceramides, fatty acids, and other barrier-supporting ingredients in your moisturizer or serum.
One particularly interesting combination involves using red light therapy alongside wet wrap therapy. Wet wraps involve applying moisturizer to damp skin, then covering with a damp layer and a dry layer to enhance hydration.
Adding red light exposure after the wraps come off might extend and enhance the barrier benefits you get from the wrapping protocol.
Common Mistakes That Undermine Results
The biggest mistake people make with red light therapy is inconsistency. They’ll use it enthusiastically for a few weeks, see minimal change, and abandon it.
But the clinical trials that documented improvements used protocols lasting months. The study with 81 patients ran for nearly a year with weekly treatments before researchers assessed outcomes.
Your skin doesn’t regenerate overnight. Barrier repair takes time.
Inflammatory patterns that have been established over years don’t reverse in days.
You need consistent application over weeks to months before evaluating whether red light therapy is working for your particular case.
Another common error is using red light during active flares despite recommendations to avoid that timing. I understand the impulse; when your skin is intensely inflamed, you desperately want something that might help immediately.
But adding any stimulus to severely compromised skin, even non-chemical light exposure, risks worsening irritation. The patience to wait for remission before starting red light therapy really pays off in reduced negative reactions.
Inadequate power density represents a third problem. Not all LED devices are created equal.
Some emit such low power that you’d need impractically long exposure times to match the parameters used in clinical studies.
When selecting a device, look for specifications that include power output measured in milliwatts per square centimeter. Higher quality devices typically provide this information clearly.
Expecting red light therapy to work as a standalone treatment sets you up for disappointment. Even the researchers who documented significant improvements emphasized that light therapy should complement, not replace, established eczema management.
Continue your moisturizer routine. Keep prescribed medications available for flares.
Red light works as an enhancement to your existing protocol.
Some people use red light therapy on unclean skin. If you’ve got moisturizer residue, sweat, or environmental debris on your skin, that can interfere with light penetration. Cleanse gently before treatment sessions to maximize the light that actually reaches your cells.
Another mistake involves inconsistent treatment areas. If you have eczema on your hands, inner elbows, and behind your knees, you need to treat all affected areas consistently.
Some people focus on the most visible areas and neglect others, then wonder why they’re not seeing comprehensive improvement.
Key Takeaways
Red light therapy works through enhanced mitochondrial function and ATP production, giving cells more energy for the repair processes that are compromised in eczema.
Multiple clinical trials show measurable improvements in inflammation, barrier function, and eczema severity markers with consistent use over weeks to months.
Timing matters tremendously; red light therapy works best during remission periods for prevention and barrier strengthening as opposed to during active inflammatory flares.
The intervention shows greatest benefit as an adjunctive treatment complementing established eczema management approaches like moisturizers and prescription medications.
Consistency over months decides whether you’ll see meaningful results, requiring patience and systematic tracking to assess effectiveness properly.
Device selection should match your specific needs based on eczema distribution, with wavelengths in the 600-700 nanometer range for red light and potentially extending to near-infrared for deeper penetration.
The remarkably favorable safety profile with minimal documented side effects makes red light therapy a low-risk addition to comprehensive eczema protocols, particularly valuable for those seeking to minimize systemic medication use or topical steroid application.
Ready to get started? See our full list of affordable and effective red light therapy devices for at-home use here.
People Also Asked
Does red light therapy help with eczema?
Yes, multiple clinical studies have shown that red light therapy can improve eczema symptoms when used consistently over weeks to months. Red light in the 600-700 nanometer range helps reduce inflammation, strengthen skin barrier function, and decrease common eczema symptoms like redness, roughness, and flaking.
The mechanism works through enhanced mitochondrial function, which gives skin cells more energy for repair processes.
Red light therapy works best during remission periods as opposed to during active flares, and it should complement as opposed to replace, standard eczema treatments.
What wavelength of red light is best for eczema?
The optimal wavelength range for treating eczema is 600-700 nanometers for red light, with some additional benefit from near-infrared wavelengths in the 700-1100 nanometer range. Red light at these wavelengths penetrates past the epidermis to reach cells in the dermis, where it can influence inflammatory processes and barrier repair.
Many effective devices mix both red and near-infrared wavelengths, as research suggests this combination may produce better results than either wavelength alone.
The specific wavelength matters because different wavelengths penetrate to different depths and interact with cellular structures differently.
How often should I use red light therapy for eczema?
The research shows benefits from frequencies ranging from once weekly to daily treatments. A conservative starting point is 2-3 times per week for 10 minutes per session, gradually increasing frequency based on how your skin responds.
Some clinical studies used just once-weekly treatments for two minutes and still documented improvements, though more frequent protocols typically show faster results.
The key is consistency over months as opposed to intensity over days. You’re looking for gradual barrier strengthening and inflammation reduction, which takes time regardless of treatment frequency.
Can I use red light therapy during an eczema flare?
Dermatologists generally recommend avoiding red light therapy during active eczema flares. During flares, your skin barrier is severely compromised, and your immune system is already in overdrive.
Adding any stimulus to this vulnerable state, even useful light exposure, can potentially cause additional irritation.
Red light therapy works best during remission periods when inflammation has calmed down, but barrier function stays impaired. Using it preventively during remission helps strengthen your skin and may reduce the frequency or severity of future flares.
Does red light therapy reduce skin inflammation?
Yes, red light therapy has been shown to reduce skin inflammation through several mechanisms. Research shows that red and near-infrared light modulates pro-inflammatory cytokines, those chemical messengers that drive inflammatory responses in conditions like eczema.
Studies have documented reduced levels of IL-4, IL-13, and IL-31, cytokines specifically associated with atopic dermatitis.
Red light also appears to stabilize mast cells and reduce their degranulation, which decreases histamine release and subsequent inflammation. These anti-inflammatory effects typically manifest over weeks of consistent treatment as opposed to immediately.
What type of red light device is best for eczema?
The best device type depends on where your eczema appears on your body. For localized patches on hands, elbows, or small areas, a handheld wand provides targeted treatment.
For facial eczema, an LED mask offers convenient full-face coverage with built-in eye protection.
For widespread eczema affecting large body areas, a panel system is more practical despite the higher cost. Look for devices that clearly specify wavelength output in the 600-700 nanometer range, power density of at least 20-40 mW/cm², and treatment distance recommendations.
Avoid devices that don’t provide technical specifications.
Can red light therapy replace steroid creams for eczema?
Red light therapy should not replace steroid creams or other prescribed medications for eczema management. The clinical evidence shows red light works best as an adjunctive treatment that complements standard therapies.
That said, consistent red light therapy during remission periods may help reduce how often you need to use topical steroids by preventing flares and maintaining barrier function between flares.
Some people find they can use lower doses of maintenance medications when combining them with regular red light therapy, but any medication adjustments should be made under a dermatologist’s supervision.
How long does it take to see results from red light therapy for eczema?
Most clinical studies showing positive results used treatment protocols lasting 8-12 weeks before assessing outcomes, with some studies continuing for nearly a year.
You might notice subtle improvements in skin texture or reduced inflammation within 4-6 weeks of consistent treatment, but significant barrier repair and symptom reduction typically require at least 2-3 months of regular application.
The timeline varies based on eczema severity, treatment frequency, and the person’s response.
This is why tracking progress with photos and symptom logs helps; improvements often happen gradually enough that you might not notice day-to-day changes.
This article includes affiliate links. If you click through and make a purchase, I may receive a small commission. This helps support the site and allows me to keep creating helpful content at no extra cost to you.